
Our Office
Visit Us Online
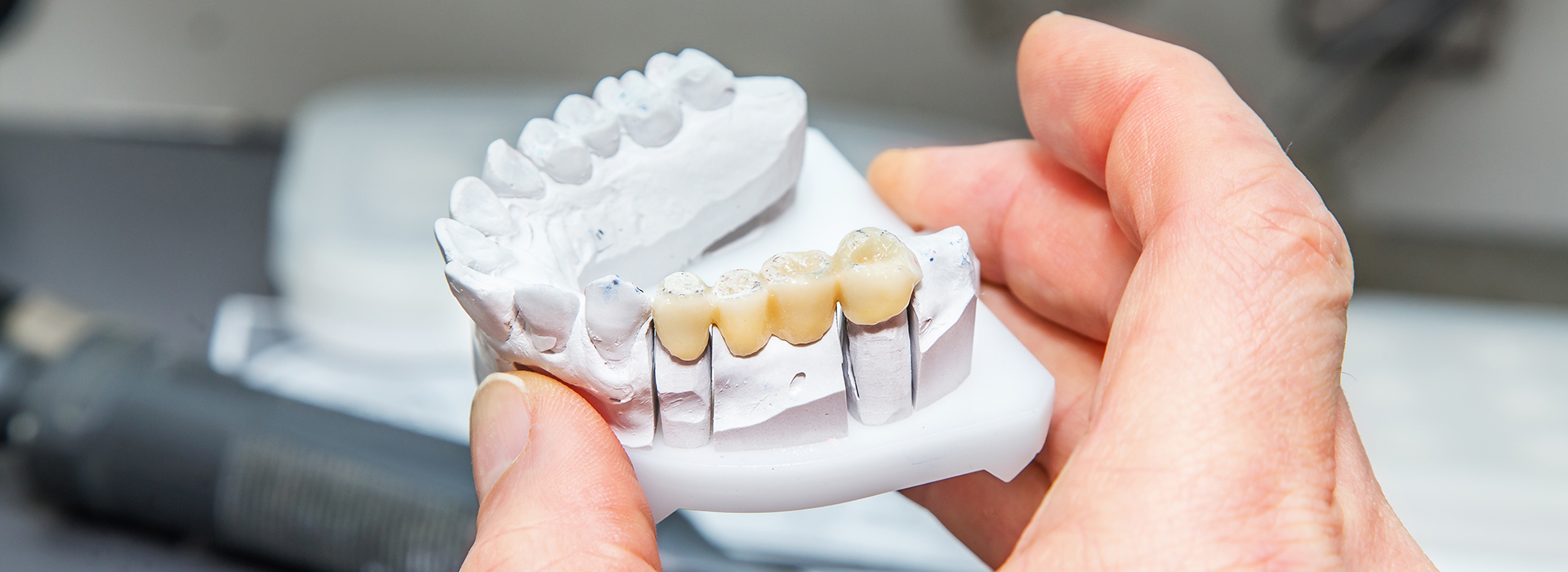
At Frisco Smiles Dentistry, we help patients restore healthy, reliable smiles after tooth loss. Missing teeth affect more than appearance — they change how your mouth functions, how your bite distributes force, and how easy it is to care for the remaining teeth. Our approach is to evaluate each case carefully and recommend durable, well-fitting bridgework when it best meets a patient’s needs and goals.
When a tooth is lost, the space it leaves behind creates ripple effects in the rest of the mouth. Adjacent teeth tend to drift or tilt toward the open space, which can alter the way your teeth fit together and create uneven wear. Over time these shifts may make chewing less efficient and can increase strain on other teeth.
Changes in occlusion (how your teeth contact when you bite) may also lead to jaw discomfort, increased sensitivity, or more frequent dental problems because misaligned teeth are harder to clean properly. In addition, missing teeth in one arch can allow opposing teeth to over-erupt, further compromising bite alignment and function.
Beyond the mechanical effects, missing teeth can change facial support and muscle function. Restoring those lost teeth with an appropriate replacement helps preserve chewing ability, supports normal facial contours, and protects the long-term health of the surrounding teeth and jawbone.
Dental care offers a spectrum of tooth-replacement options, each suited to different clinical situations and patient priorities. Bridges are a reliable midline solution when neighboring teeth can provide support or when implants are used as anchors. They restore a continuous biting surface, which makes eating and speaking feel more natural again.
Choosing the right option depends on the number and location of missing teeth, the condition of the remaining teeth and bone, and the patient’s oral hygiene habits and expectations for longevity. A well-planned restoration re-establishes function while minimizing harm to healthy tooth structure whenever possible.
Our goal is to recommend a treatment that balances durability and aesthetics, so your replacement looks natural and performs comfortably for years. We take time to explain the pros and cons of each approach so you can make an informed decision that fits your lifestyle.
A dental bridge is a fixed restoration that replaces one or more missing teeth by spanning the gap with artificial teeth (pontics) that are anchored to support structures. Those supports can be natural teeth that are prepared for crowns or implants placed in the jaw. Because a bridge is fixed in place, patients experience stable chewing and a consistent appearance without the need to remove the restoration.
Bridges protect the alignment of the remaining teeth by filling the empty space and preventing neighboring teeth from shifting. They also restore contact points and chewing surfaces that help distribute the forces of biting evenly across the arch, which reduces the risk of overloading individual teeth.
Modern bridge materials—such as high-strength ceramics and tooth-colored restorations—allow us to match translucency and shade closely to surrounding teeth, delivering results that are both functional and attractive while resisting staining and wear.
There are several bridge designs, and the right one depends on the clinical context. A traditional fixed bridge uses crowns on the teeth adjacent to the gap to support one or more pontics. This design is dependable when the abutment teeth are healthy enough to support the crowns.
A cantilever bridge anchors the pontic to a crown on only one adjacent tooth. This approach is useful in situations with space or anatomical limitations, but it places more load on a single supporting tooth and is chosen selectively.
Maryland (resin-bonded) bridges use a metal or ceramic framework bonded to the back of adjacent teeth. They conserve tooth structure because the adjacent teeth typically require less preparation, making this a conservative choice for certain front-tooth replacements.
Implant-supported bridges rely on dental implants as the anchors rather than natural teeth. Because implants integrate with bone and act like tooth roots, they can support larger restorations without involving neighboring teeth, and they help preserve jawbone volume over time.
Successful bridge treatment begins with a thorough evaluation of oral health. That includes assessing gums, the stability and condition of adjacent teeth, bite relationships, and the quality of the underlying bone. Any active gum disease or untreated decay must be addressed first to provide a healthy foundation for a bridge.
If the abutment teeth are weakened by large fillings or decay, they may need additional treatment such as root canal therapy or buildup work before crowns can reliably support a bridge. In cases intended for implant support, we evaluate bone volume and density to determine whether grafting or other preparatory procedures are necessary.
Treatment planning often involves digital imaging and precise impressions so the final restoration fits accurately and restores an appropriate bite. Proper diagnosis and preparation improve long-term outcomes and reduce the likelihood of complications after placement.
The process for a traditional bridge usually spans several visits. After a comprehensive diagnostic appointment, the supporting teeth are prepared by removing a small amount of enamel to accommodate crowns. An impression or digital scan captures the prepared teeth so a lab can fabricate the custom bridge.
A temporary bridge is placed to protect the prepared teeth and maintain function and aesthetics while the permanent restoration is being made. Temporary restorations allow you to test the shape and feel of the new teeth so adjustments can be made before the final bridge is cemented.
When the permanent bridge returns from the lab, we verify the shade, contours, and how the restoration contacts neighboring teeth. After fine-tuning the fit and bite, the bridge is secured with durable dental cement. Post-placement care includes instruction on cleaning under and around the pontics and attending regular checkups to monitor the restoration and supporting teeth.
Implant-supported bridges begin with surgical placement of implants into the jawbone. We use precise imaging to plan implant position for optimal support and long-term success. The surgery is performed on an outpatient basis with local anesthesia and, when appropriate, sedation options to keep patients comfortable.
After placement, implants need time to integrate with the bone. This healing period—known as osseointegration—typically takes several months and ensures the implants become stable anchors for the final bridge. In many cases, a temporary restoration can be used during healing to provide aesthetics and function without stressing the healing sites.
Once integration is complete, the implant-supported bridge is fabricated and attached. Because implants stimulate the jawbone similarly to natural teeth, this approach helps maintain facial support and reduces the bone loss that can follow tooth loss. Follow-up visits focus on monitoring healing, checking occlusion, and confirming the restoration’s comfort and performance.
Whether you are considering a traditional bridge, an implant-supported solution, or need guidance on the best way to restore a missing tooth, our team is here to help. Contact us to learn more about restoring your smile and to schedule a consultation to discuss which option fits your goals and oral health needs.
A dental bridge is a fixed prosthesis that replaces one or more missing teeth by spanning the gap with artificial teeth called pontics. The pontics are attached to support structures, which may be natural teeth prepared for crowns or dental implants placed in the jaw. Because a bridge is secured in place, it restores a continuous biting surface and helps return normal chewing and speech function.
Bridges also preserve the position of neighboring teeth by filling the empty space and preventing unwanted drifting or tipping. Restoring contact points and occlusion helps distribute bite forces more evenly across the arch, reducing stress on individual teeth. Modern materials allow bridges to match surrounding teeth in shade and translucency for a natural appearance.
Common designs include traditional fixed bridges, cantilever bridges, Maryland (resin-bonded) bridges, and implant-supported bridges. A traditional fixed bridge uses crowns on teeth adjacent to the gap as abutments, while a cantilever attaches to only one adjacent tooth and is used selectively when space or anatomy limits options. Maryland bridges use a metal or ceramic framework bonded to the backs of adjacent teeth to conserve tooth structure, most often for front-tooth replacements.
Implant-supported bridges rely on dental implants as anchors rather than natural teeth, allowing larger spans without involving adjacent teeth. Each design has specific clinical indications based on tooth location, abutment health, and the size of the gap. Your dentist will recommend the design that best balances durability, function, and conservation of healthy tooth structure.
A good candidate for a dental bridge has one or more missing teeth with healthy adjacent teeth or adequate jawbone for implant placement. Candidates should have controlled gum disease and good oral hygiene habits because the long-term success of a bridge depends on the health of supporting tissues. The location of the missing tooth, bite relationships, and overall dental health also influence suitability.
Patients with extensive decay or weakened abutment teeth may need additional treatments such as buildups or root canal therapy before a bridge can be placed. When natural teeth are not suitable abutments, implant-supported bridges can be considered if bone volume is sufficient or can be augmented. A thorough evaluation and imaging help determine the safest and most predictable option for each patient.
Preparation begins with a comprehensive exam to evaluate the health of the gums, the condition of adjacent teeth, bite alignment, and underlying bone. Any active decay or periodontal disease must be treated first to create a stable foundation for the restoration. When the abutment teeth are ready, the dentist shapes them by removing a small amount of enamel to make room for crowns that will support the bridge.
After preparation, a digital scan or impression captures the prepared teeth and bite relationships so the lab can fabricate the custom bridge. A temporary bridge is placed to protect the prepared teeth and maintain function and aesthetics while the permanent restoration is made. Once the final bridge returns from the lab, the dentist verifies fit, shade, and occlusion before cementing it in place.
Implant-supported bridge treatment begins with surgical placement of implants into the jawbone at planned positions to support the restoration. The procedure is performed under local anesthesia, often with sedation options available to improve comfort, and precise imaging guides implant placement for optimal alignment and load distribution. After surgery, a healing period is required to allow the implants to integrate with the bone, a process called osseointegration.
Osseointegration typically takes several months depending on the individual and the location in the jaw, and temporary restorations may be used during this time to maintain function and appearance. Once integration is complete, the final bridge is fabricated and attached to the implant abutments, then adjusted for proper bite and comfort. Follow-up appointments monitor healing, occlusion, and the integrity of the restoration.
The lifespan of a dental bridge varies, commonly lasting many years when proper oral hygiene and routine dental care are maintained. Material selection, the quality of the fit, and the health of the supporting teeth or implants strongly influence longevity. Habits such as grinding or clenching, poor oral hygiene, and untreated gum disease can shorten a bridge’s functional life.
Regular professional cleanings and periodic dental exams help detect early issues such as decay at the margins, loosening of cement, or changes in bite that can compromise the restoration. When problems are identified early, repairs or adjustments can often be made to extend the bridge’s service. Implant-supported bridges may preserve bone and offer different longevity considerations compared with tooth-supported designs.
Daily cleaning under and around the pontics is essential to prevent plaque buildup and maintain the health of supporting tissues. Use a floss threader or interdental brush to clean beneath the bridge, and consider a water flosser if recommended by your dentist to flush debris from hard-to-reach areas. Continue twice-daily brushing with a fluoride toothpaste and pay special attention to the margins where crowns meet tooth structure.
Avoid using the bridge as a tool and minimize habits that place excessive force on the restoration, such as biting very hard or chewing nonfood items. Maintain regular dental visits so your clinician can professionally clean around the bridge and evaluate its fit and the health of abutment teeth. Prompt attention to sensitivity, loosening, or discomfort helps prevent more extensive problems.
Complications can include decay of abutment teeth, loosening or failure of the cement bond, fracture of the pontic or framework, and periodontal problems if plaque control is inadequate. Over time, changes in the supporting teeth or jawbone can alter how a bridge fits, leading to gaps, food trapping, or bite changes that require professional evaluation. Cantilever designs and improperly distributed forces can place additional stress on a single abutment, increasing risk in certain situations.
Early detection through routine exams reduces the chance of severe complications and may allow repairs rather than replacement. When abutment teeth fail, alternative solutions such as implant-supported restorations may become necessary. Your dentist will discuss risk factors specific to your mouth and recommend strategies to minimize those risks before treatment begins.
Dental bridges, implants, and removable dentures each have distinct clinical advantages and considerations depending on a patient’s oral health and treatment goals. Bridges provide a fixed, natural-feeling restoration when adjacent teeth can serve as supports or when implants are available as anchors, and they often require less surgical intervention than full-arch implant solutions. Dental implants preserve bone by replacing the tooth root and avoid altering neighboring teeth, while removable dentures offer a noninvasive, reversible option for replacing multiple teeth.
The choice among these options depends on factors such as bone volume, the condition of neighboring teeth, desired permanence, and the patient’s oral care routine. A careful evaluation helps identify which solution offers the best balance of function, aesthetics, and conservation of healthy structures. Your dentist can explain the trade-offs and likely outcomes so you can choose an approach aligned with your needs.
To begin, schedule a consultation at Frisco Smiles Dentistry where the team will review your dental history, perform an oral exam, and take any necessary imaging such as digital radiographs or scans. The dentist will assess the health of your gums, the condition of neighboring teeth, bite relationships, and bone volume to determine whether a traditional or implant-supported bridge is most appropriate. This visit focuses on diagnosis, discussing options, and outlining next steps tailored to your oral health and goals.
If additional treatments are required to prepare the site—such as addressing decay, treating gum disease, or performing bone grafting—those will be planned before bridge placement to maximize long-term success. The team will explain the proposed timeline, what to expect during each phase, and how to care for the site during healing. A personalized treatment plan gives you a clear path forward and ensures the restoration supports both function and appearance.
