Our Office
Visit Us Online
When decay or minor damage affects a tooth, composite (tooth-colored) fillings restore both appearance and function without drawing attention to the repair. Modern composite resins are engineered to mimic the translucency and shade of natural enamel, allowing clinicians to match a restoration to the surrounding dentition for a seamless result. Beyond cosmetics, composites provide a durable surface that withstands normal chewing forces when placed properly.
These restorations are composed of a resin matrix combined with glass or ceramic fillers that improve strength and polishability. Because composites can be precisely shaded and sculpted, they are the material of choice for visible teeth and for patients who prefer metal-free solutions. The technique relies on bonding chemistry rather than mechanical retention, so the final restoration appears and feels more like the original tooth.
At Frisco Smiles Dentistry, our approach to composite fillings emphasizes long-term stability and natural aesthetics. We evaluate each restoration on its own merits—considering the size of the defect, the location in the mouth, and the patient’s bite—to recommend a conservative solution that preserves as much healthy tooth structure as possible while restoring normal form and function.
Choosing a tooth-colored filling lets patients regain a confident smile without the visual compromise of metal restorations. These materials are versatile, repairable, and compatible with other restorative options should needs change in the future.
One of the primary advantages of composite fillings is the adhesive bond formed with enamel and dentin. Unlike older restorations that required extensive shaping of the tooth for mechanical retention, adhesive techniques allow clinicians to remove only the diseased tissue and leave healthy structure intact. That conservative approach strengthens the remaining tooth and reduces the need for more extensive treatment later on.
The bonding process also seals the margin between the filling and the tooth, helping to limit microleakage and reducing the risk of recurrent decay when combined with good oral hygiene. Because less natural tooth is sacrificed during preparation, composite restorations can often be repaired or replaced with minimal additional removal of tooth material, which is an important consideration for long-term oral health.
Composites are also versatile in their application. They can restore small to moderate cavities, repair chipped enamel, and close minor gaps in certain circumstances. When clinical conditions require a stronger, more extensive restoration, alternatives such as inlays, onlays, or crowns may be recommended—but for many defects, bonded composites strike an effective balance between conservation and durability.
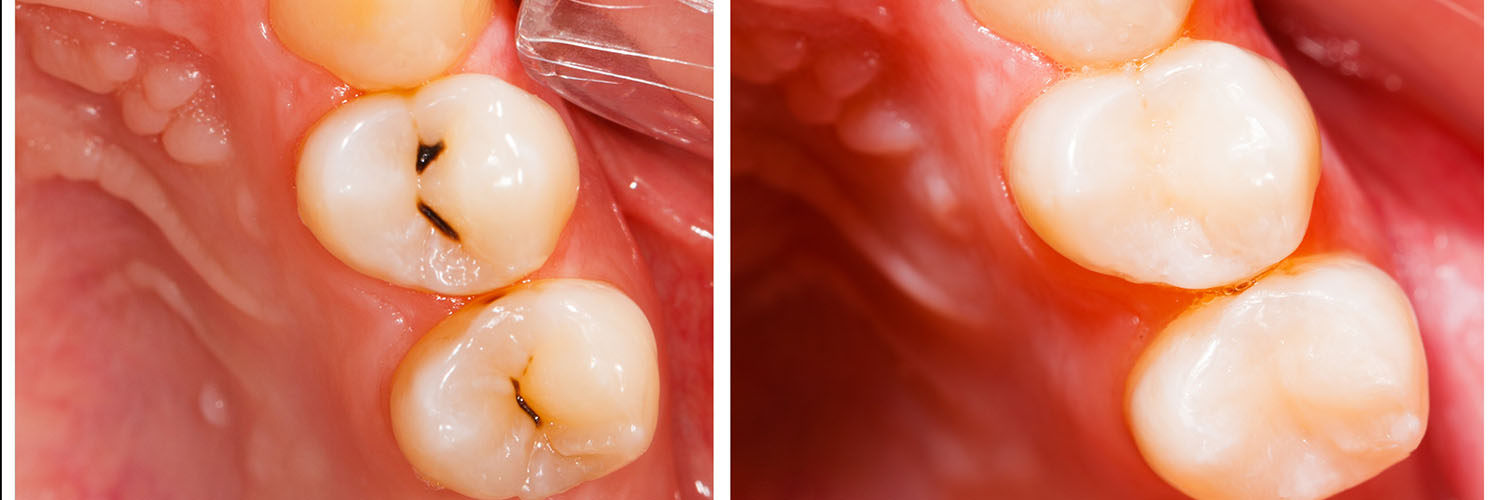
A typical filling appointment is straightforward and designed with patient comfort in mind. After a thorough exam and discussion of options, the tooth is isolated and the decayed or weakened tissue is carefully removed. Local anesthesia is used as needed to ensure the procedure is painless; many patients find the process quick and minimally invasive when performed by an experienced clinician.
Once the tooth is prepared, the bonding protocol begins. The tooth surface is conditioned, the adhesive system is applied, and the composite resin is placed incrementally. Layering the material in small increments helps control polymerization shrinkage and lets the clinician contour the restoration to match the tooth’s natural anatomy. Each layer is set with a curing light before the next is added.
After sculpting the final anatomy, the filling is polished and the bite is checked and adjusted so the restoration feels comfortable during chewing. Most composite fillings are completed in a single visit, and clinicians will review homecare and any temporary sensitivity to expect in the days following treatment. For patients who experience dental anxiety, we offer supportive measures and discuss options such as nitrous oxide or oral sedation to help you feel relaxed during care.
Immediately after treatment it is normal to have temporary numbness from local anesthesia; avoid chewing or biting on the treated side until sensation returns to prevent soft-tissue injury. Mild sensitivity to temperature or biting forces can occur for a few days as the tooth adjusts; this generally subsides on its own but should be reported if it is severe or persists beyond a couple of weeks.
Long-term success depends on maintaining a clean environment around the restoration. Routine brushing with fluoride toothpaste, daily interdental cleaning, and regular dental examinations help detect and prevent recurrent decay. If you notice roughness, discoloration, or a change in how your bite feels, schedule an appointment so the restoration can be evaluated and, if necessary, refined or repaired.
Composite materials are resilient, but they are not indestructible. Avoid using teeth as tools and be mindful of habits that place excessive force on restorations—such as hard chewing, ice chewing, or opening packages with your teeth. For patients who habitually grind or clench, a protective nightguard can reduce wear and extend the life of restorations.
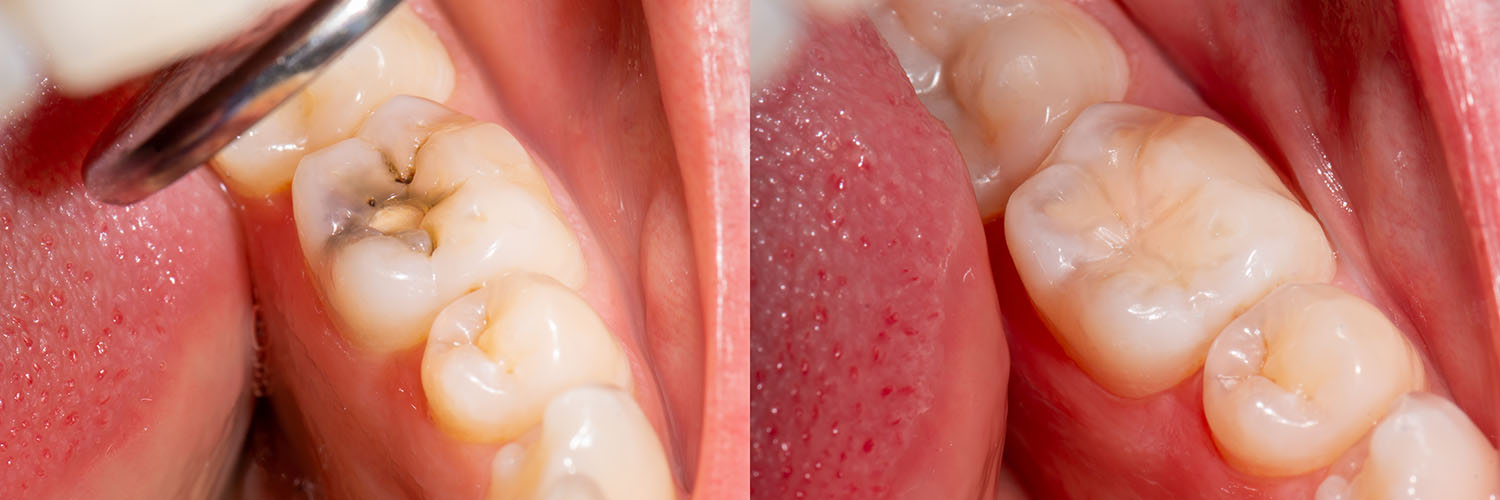
Not every defect is suitable for a direct composite filling. Large areas of decay, cracks that extend into the root, or extensive tooth loss may call for indirect restorations—such as inlays, onlays, or full-coverage crowns—or for endodontic treatment if the pulp is involved. Your clinician will evaluate the tooth’s prognosis and present options that balance durability, aesthetics, and preservation of tooth structure.
Follow-up is an important part of that decision-making process. Regular checkups and radiographs allow your dental team to monitor restorations and identify early signs of failure, recurrent decay, or structural compromise. When detected early, many problems can be managed conservatively; when more extensive treatment is necessary, timely care helps prevent loss of the tooth and limits the need for emergency interventions.
When a replacement is recommended, modern indirect materials provide excellent longevity and esthetics. The goal is always to restore comfort and function while planning for the tooth’s long-term health. Open communication about risks, benefits, and expected outcomes helps patients make confident decisions about their restorative care.
At Frisco Smiles Dentistry, our priority is restoring teeth in a way that maintains both appearance and long-term oral health. If you have questions about composite fillings or which restorative option is best for your situation, please contact us for more information.
Composite fillings are tooth-colored restorations made from a resin matrix combined with glass or ceramic fillers that mimic the shade and translucency of natural enamel. They are placed using adhesive bonding protocols that attach the material to enamel and dentin, which allows for more conservative removal of decayed tissue. Because composites are shaded and sculpted to match surrounding teeth, they restore both appearance and function without the metallic look of older materials.
Unlike traditional metal (amalgam) restorations that rely on mechanical retention, composite restorations bond to the tooth structure and preserve more healthy enamel and dentin. This adhesive approach often improves the long-term strength of the remaining tooth and reduces the need for extensive preparation. Composites are also repairable in many cases, making them a versatile option for visible areas of the mouth.
Composite fillings are well suited for small to moderate cavities, cosmetic repairs such as chipped enamel, and situations where a metal-free restoration is preferred. Clinicians consider the size and location of the defect, the tooth's role in chewing, and the patient’s bite when recommending a composite. For many front and premolar teeth, composites provide an excellent balance of aesthetics and durability.
Large areas of decay, cracks that extend below the gumline, or teeth with extensive structural loss may require indirect restorations such as inlays, onlays, or crowns. Your dentist will evaluate radiographs and clinical findings to determine whether a direct composite is appropriate or if a stronger, laboratory-fabricated restoration would offer a better long-term prognosis. The goal is always to preserve as much healthy tooth as possible while restoring function and comfort.
A typical appointment begins with a thorough exam and discussion of options, followed by isolation of the tooth and removal of the decayed or weakened tissue with precision instruments. Local anesthesia is used as needed to ensure comfort, and many patients find the procedure quick and minimally invasive when performed by an experienced clinician. The prepared tooth is conditioned and a bonding system is applied before the composite material is placed.
The composite is layered incrementally, with each layer cured by a light to control shrinkage and build proper anatomy. Once the restoration is sculpted, the dentist will check and adjust the bite, then polish the surface to a natural luster. Most direct composite fillings are completed in a single visit, and your clinician will review what to expect in the days after treatment.
Composite fillings can function effectively for many years, but their longevity depends on several factors including the size and location of the restoration, the quality of placement, and the patient’s oral hygiene habits. Restorations placed on teeth that endure heavy chewing forces or that are subject to grinding may wear faster than those in low-stress areas. The skill of the clinician and attention to bonding technique also play important roles in long-term performance.
Maintaining routine dental examinations, practicing diligent oral hygiene, and addressing habits that place excessive force on teeth will help extend the life of a composite restoration. When problems such as marginal staining, roughness, or recurrent decay are detected early, many restorations can be repaired conservatively. Timely professional care and preventive measures support the durability of restorations over time.
Mild sensitivity to temperature or biting pressure is common for a few days after a filling as the tooth adjusts to the restoration, and it typically subsides without intervention. This short-term sensitivity is often related to the bonding process, the proximity of the decay to the nerve, or minor inflammation of the tooth structure. Over-the-counter analgesics and avoiding extreme temperatures for a short period usually provide adequate relief.
If sensitivity is severe, worsens, or persists beyond a couple of weeks, you should contact your dental team for evaluation as it may indicate deep decay, a high spot that needs adjustment, or involvement of the tooth’s pulp. In some cases additional treatment such as a revision of the restoration or endodontic therapy may be necessary to address the underlying cause. Prompt assessment helps preserve the tooth and prevent complications.
After receiving a composite filling, avoid chewing on the treated side until local anesthesia wears off to prevent soft-tissue injury, and be gentle with the tooth while it acclimates. Maintain thorough oral hygiene with twice-daily brushing using fluoride toothpaste and daily interdental cleaning to reduce the risk of recurrent decay at the margins. A balanced diet that limits frequent exposure to sugary and acidic foods supports the health of restorations and surrounding teeth.
Regular dental checkups allow your clinician to monitor the restoration’s condition and make minor refinements if needed, which can extend its service life. If you have habits that place extra stress on teeth—such as grinding, clenching, or biting hard objects—discuss protective measures like a custom nightguard with your dentist. Early attention to changes in bite, texture, or color helps keep restorations functioning well.
One advantage of composite materials is their reparability; small chips, marginal defects, or localized wear can often be corrected without removing the entire restoration. Because composites bond to tooth structure, a skilled clinician can add new material to the affected area and blend it with the existing restoration to restore form and function. Repair is generally less invasive than full replacement and helps conserve remaining tooth structure.
When damage is extensive, recurrent decay is present, or the restoration no longer provides a predictable seal, replacement may be the better option to restore the tooth’s integrity. Your dentist will assess the condition of the restoration, evaluate surrounding tooth structure, and recommend the most conservative yet durable solution. Open communication about risks and expected outcomes ensures a treatment plan suited to long-term oral health.
Composite resins are widely used and considered safe for the majority of patients; they have been subjected to extensive research and clinical use over many decades. Modern materials are cured in the mouth to form a stable matrix, and clinicians select products based on proven performance and biocompatibility. Patients with specific material sensitivities or allergies should inform their dental team so alternative materials can be discussed.
If you have questions about the composition of restorative materials or potential systemic effects, your dentist can explain the evidence and address individual concerns. Open discussion helps align treatment choices with your health history and preferences while ensuring restorations meet clinical goals for function and appearance. Practitioners follow best practices to minimize exposure and maximize the safety of dental procedures.
Alternatives to direct composite fillings include amalgam, glass ionomer, and indirect restorations such as laboratory-fabricated inlays, onlays, and crowns. Indirect restorations are often recommended when a cavity is large, when substantial tooth structure has been lost, or when additional strength and coverage are needed to restore long-term function. Each option has distinct properties related to strength, wear resistance, and suitability for different locations in the mouth.
Your dentist will review the pros and cons of each material and restoration type based on the tooth’s condition, aesthetic priorities, and functional demands. In some cases a staged approach—such as placing a direct restoration initially and monitoring its performance—may be appropriate before recommending a more extensive restoration. The decision prioritizes preservation of tooth structure and predictable outcomes.
At Frisco Smiles Dentistry the restorative decision starts with a comprehensive evaluation that includes a clinical exam, review of your oral health history, and radiographs when indicated to assess the extent of decay or structural damage. The clinician evaluates factors such as defect size, location, occlusion, restorative history, and long-term prognosis to weigh conservative and durable options. Patient preferences regarding aesthetics, treatment time, and maintenance also play an important role in the final recommendation.
After discussing the likely outcomes, risks, and benefits of each option, your clinician will recommend a treatment plan that aims to preserve healthy tooth structure while restoring comfort and function. Regular follow-up and preventive care are integrated into the plan to monitor restorations over time and address concerns early. This collaborative approach helps patients make informed choices aligned with their oral health goals.
