
Our Office
Visit Us Online
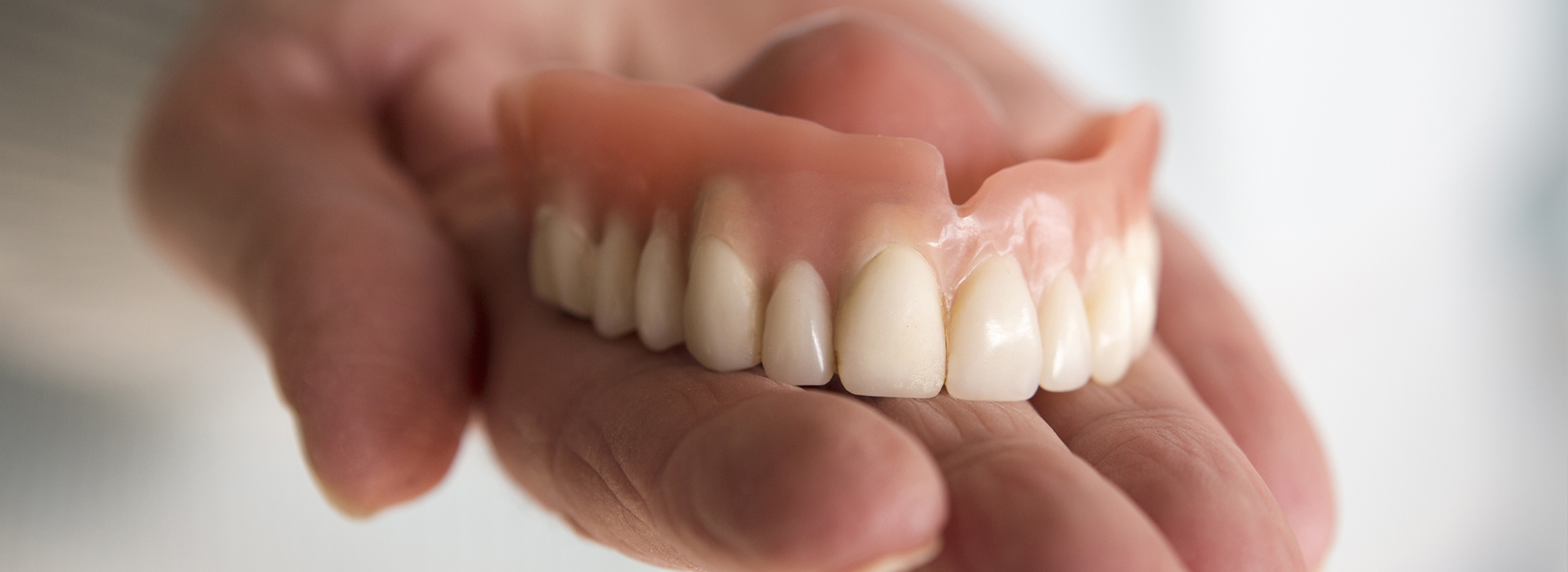
Advances in dental materials and prosthetic design have made replacing missing teeth more natural, comfortable, and long-lasting than ever before. While fixed solutions such as dental implants and bridgework are excellent options for many patients, removable dentures remain a reliable choice for restoring function, facial support, and a confident smile.
At the office of Frisco Smiles Dentistry, we take a detailed, patient-centered approach to denture care. Our team focuses on precise fit, proper bite alignment, and a lifelike appearance so each appliance performs well and complements your facial features.
We tailor every denture to each person's needs, considering oral health, lifestyle, and long-term goals. The result is a restoration that helps you speak, eat, and smile with greater ease while preserving oral comfort and the health of remaining tissues.
Losing teeth does more than create an empty space where a tooth once stood. Tooth loss changes how forces are distributed across the bite, which can cause neighboring teeth to shift and change position over time. Those shifts may create new gaps, alter chewing efficiency, and complicate future restorative options.
Beyond mechanical changes, missing teeth also affect soft tissue and bone. Without normal stimulation from chewing, the jawbone slowly remodels and may lose volume, which in turn can make the face appear sunken or aged. Restoring teeth with a well-fitting denture helps reinstate support for lips and cheeks, improving overall facial proportions.
There are also everyday consequences to consider. Speech can be affected, and certain foods may become difficult to eat, which can affect nutrition and enjoyment of meals. Addressing missing teeth sooner rather than later often makes it easier to preserve oral health and achieve the most comfortable long-term result.
Dentures are removable prosthetic teeth set into a supportive base that rests on the gums. The base is designed to follow the contours of the mouth so the appliance feels secure and looks natural. Dentures can replace a few missing teeth or an entire arch, depending on the individual case.
Because dentures are removable, they offer the advantage of easy cleaning for both the appliance and the tissues beneath it. Proper daily hygiene—brushing the prosthesis and cleaning the gums and any remaining teeth—helps maintain oral health and prolongs the life of the denture.
Modern denture materials mimic the translucency and shade of natural teeth while the base materials are engineered for comfort and durability. When designed with attention to bite relationships and facial balance, a denture can restore effective chewing, clearer speech, and an appearance that supports a natural smile.
Choosing among denture options starts with a careful clinical examination, including evaluation of remaining teeth, gum health, and bone structure. Our approach emphasizes finding a solution that matches your functional needs and daily routine while minimizing future complications.
Two broad categories of removable prostheses are full (complete) dentures and partial dentures. Full dentures replace all teeth in an arch, while partials fill in gaps left by one or more missing teeth and rely on remaining teeth for support and stabilization.
Some patients benefit from hybrid approaches that combine removable prostheses with implants or attachments for improved retention. These combinations can dramatically increase stability and chewing efficiency while still offering the maintenance advantages of a removable appliance.
Complete dentures restore all teeth in the upper or lower jaw. The design varies among patients; careful attention to the bite and tooth arrangement is essential to achieve comfortable function and a pleasing appearance. Planning includes selecting tooth shape, shade, and positioning for a lifelike result.
An immediate denture is placed at the time of extractions so the patient leaves the appointment with teeth in place. While convenient, immediate prostheses commonly require adjustments or relines as tissues heal and change shape. In contrast, a conventional denture fabricated after healing can provide a more stable fit from the start.
Overdentures and retained roots
Overdentures can gain stability by using remaining tooth roots or special attachments that preserve bone and improve retention. This approach can be beneficial for patients who want greater support without committing to a full implant-retained restoration.
Implant-assisted dentures
When implants are strategically placed, a removable denture can clip or snap onto those implants for substantial improvements in stability and comfort. Implant attachments reduce movement during chewing and speech and can enhance confidence with daily activities.
Partial dentures are designed to replace select missing teeth while integrating with the remaining dentition. They can prevent adjacent teeth from drifting into empty spaces and help maintain the overall alignment and function of the bite.
Partial frameworks come in a variety of materials—cast metal, flexible resins, or hybrid constructions—so the selected design balances strength, comfort, and aesthetics. Precision attachments or discreet clasps are used to secure the partial while keeping it as inconspicuous as possible.
When planning a partial denture, preserving the health of the teeth that will support the appliance is a priority. Careful assessment and conservative preparations help ensure the partial performs well and protects the integrity of the remaining dentition.

Creating a comfortable, well-fitting denture requires a sequence of clinical steps: a thorough exam, diagnostic records, impressions, bite records, try-ins, and final delivery. Attention at each step improves fit and reduces the need for extensive adjustments later.
Diagnostic imaging and careful evaluation of the jaw relationships help ensure the denture supports healthy oral function. When extractions or preparatory treatments are needed, the treatment plan addresses tissue healing and timing so the resulting prosthesis adapts well to the mouth.
For patients considering implant assistance, collaboration between surgical and restorative phases is important. Implant positions, restorative angulation, and attachment selection all influence the final denture design. Our team coordinates care so surgical planning and prosthetic goals are aligned for the best outcome.

Adapting to a new denture is a process. In the first days or weeks you may notice increased saliva, minor soreness in specific areas, and differences in speech or chewing. These reactions are normal and typically ease as the soft tissues adapt and small adjustments are made.
Regular follow-up visits are essential during the early adjustment period. Small relines or selective adjustments can relieve sore spots and fine-tune the bite so function and comfort improve. Your clinician will advise when to return for checks and what symptoms deserve prompt attention.
Long-term denture care includes daily cleaning of the appliance, gentle brushing of any remaining teeth and gums, and removing dentures at night to allow tissue recovery. Periodic relines or rebasing may be recommended as the jawbone and soft tissues remodel over time to maintain a secure, comfortable fit.
Practical tips for everyday wear
Start with soft foods and chew on both sides to distribute forces evenly. Read aloud or practice simple phrases to speed up speech adaptation. Rinse and brush prostheses after meals and soak them overnight as instructed.
When to seek professional help
If persistent pain, loose fit, or changes in fit occur, schedule a check so the denture can be assessed. Early attention prevents minor issues from becoming more serious and helps maintain oral health.
Follow-up exams matter
Routine dental visits allow your provider to examine soft tissues, review any remaining teeth, and confirm the ongoing suitability of the denture. These visits support the longevity of the appliance and the health of your mouth.
Our practice is committed to delivering denture care that combines technical skill with thoughtful planning and ongoing support. If you have questions about how a denture could fit into your treatment plan, please contact us for more information.
Dentures are removable prosthetic appliances that replace missing teeth and the surrounding tissues to restore chewing function and facial support. The prosthesis consists of artificial teeth set into a base that follows the contours of the mouth so it seats against the gums and distributes biting forces. When designed with attention to bite relationships and esthetics, dentures can improve speech, chewing efficiency, and the appearance of the lower face.
Modern denture materials mimic the shade and translucency of natural teeth while base materials are engineered for comfort and durability. Because dentures are removable, they allow for straightforward cleaning of both the appliance and the oral tissues beneath it. Proper fit and occlusion are essential to minimize sore spots and to maintain long-term function.
Removable dentures generally fall into two broad categories: complete (full) dentures that replace all teeth in an arch, and partial dentures that fill gaps left by one or more missing teeth. Partial dentures often rely on remaining teeth for support and can be fabricated from cast metal, flexible resin, or hybrid materials depending on the case requirements. Complete dentures are designed to restore an entire upper or lower arch and require careful attention to tooth arrangement and bite registration.
Hybrid and attachment-enhanced options also exist, such as overdentures that fit over retained roots or implant-assisted dentures that clip onto implants for improved retention. These approaches can increase stability and chewing efficiency while preserving bone and supporting facial contours. The right choice depends on oral health, bone volume, and the patient’s functional goals.
Good candidates for dentures include patients who have lost multiple teeth or an entire arch and seek to restore function, appearance, and oral support. Candidates should undergo a thorough clinical evaluation to assess gum health, remaining teeth, and bone structure so the prosthesis can be planned to minimize complications. When remaining teeth are present, preserving the health of those teeth and their supporting tissues is a priority for predictable partial denture performance.
Patients who desire enhanced stability may also be evaluated for implant-assisted solutions that combine implants with removable prostheses. The decision to proceed with a particular denture design is based on long-term goals, oral health status, and the clinical findings from diagnostic records. A coordinated treatment plan helps ensure the denture integrates well with other restorative or surgical procedures when needed.
Immediate dentures are inserted at the time of tooth extraction so the patient leaves the appointment with teeth in place, while conventional dentures are fabricated after the tissues have healed. Immediate dentures provide immediate esthetic and functional replacement but commonly require relines or adjustments as healing changes the shape of the underlying tissues. Conventional dentures often provide a more stable fit from the start because fabrication begins after healing has progressed.
When planning immediate dentures, clinicians account for anticipated tissue shrinkage and provide follow-up relines or adjustments to maintain fit. Both approaches aim to restore function and appearance, but the timeline and need for early adjustments differ. The appropriate option depends on the clinical scenario and the patient’s preferences regarding timing and interim care.
Implant-assisted dentures use dental implants strategically placed in the jaw to anchor a removable prosthesis, which significantly reduces movement during chewing and speech. Attachments such as locators, bars, or snaps allow the denture to clip onto the implants, providing improved retention compared with conventional tissue-supported dentures. This enhanced stability promotes greater comfort, more efficient chewing, and increased confidence during daily activities.
Implant-assisted options can also slow jawbone resorption by preserving bone around functional implants, helping maintain facial support over time. Treatment requires coordination between surgical implant placement and prosthetic planning so implant positions align with the final denture design. Not every patient is a candidate for implants, so a thorough evaluation determines suitability and the optimal attachment type.
Daily care for dentures includes removing the appliance at night, brushing it with a soft denture brush or nonabrasive cleanser, and rinsing it after meals to remove food debris. It is also important to gently brush the gums, tongue, and any remaining natural teeth to maintain tissue health and reduce the risk of irritation or infection. Soaking dentures overnight in a recommended solution can help disinfect the appliance and preserve its shape when not worn.
Avoid using abrasive household toothpaste or harsh chemicals that can damage denture surfaces, and handle the appliance over a sink filled with water or a folded towel to prevent breakage if dropped. Regular inspection for cracks, wear, or changes in fit helps identify issues early so they can be addressed professionally. Consistent hygiene habits extend the life of the prosthesis and support overall oral health.
The denture fitting process typically begins with a comprehensive exam, diagnostic records, and impressions to capture the shapes of the jaws and tissues. Subsequent steps include bite registration, wax try-ins to evaluate tooth position and esthetics, and final fabrication of the appliance to achieve correct occlusion and facial support. Attention to each step reduces the need for extensive adjustments after delivery.
If extractions or preparatory treatments are needed, the treatment plan will account for healing time and timing of prosthesis placement so the final denture adapts well to the mouth. Try-in appointments give the patient and clinician a chance to fine-tune appearance and function before the denture is processed. Skilled laboratory communication and clinical precision are both critical to predictable outcomes at delivery.
Adjustment to new dentures varies among individuals, but most patients experience increased saliva, minor soreness, and initial differences in speech or chewing that improve over days to weeks. Practicing with soft foods, chewing on both sides, and reading aloud to speed speech adaptation are common strategies recommended during the early period. Small, selective adjustments by the clinician often relieve sore spots and improve comfort as tissues adapt.
Persistent pain, significant difficulty eating, or ongoing stability issues warrant a prompt clinical review so the denture can be modified. Early follow-up appointments are important to track adaptation and address problems before they become more troublesome. Over time, routine relines or adjustments may be needed as the jawbone and soft tissues remodel.
Follow-up visits are essential during the initial weeks after delivery to assess fit, bite, and tissue response; clinicians typically schedule early checkups to make any necessary relines or selective adjustments. Periodic recall appointments thereafter allow the provider to monitor oral tissues, examine any remaining teeth, and confirm the ongoing suitability of the denture. Timely professional attention prevents small issues from becoming larger problems and supports long-term comfort.
Patients should also request an appointment if they experience persistent soreness, looseness, changes in speech, or visible damage to the denture. Early intervention can preserve oral health and reduce the need for more extensive corrective work. Regular exams are a key component of effective denture maintenance.
Well-designed dentures restore vertical dimension and lip support, which can improve facial proportions and reduce a sunken or aged appearance associated with tooth loss. Replacing missing teeth also helps maintain proper bite relationships and can prevent neighboring teeth from shifting into empty spaces, which preserves chewing efficiency and oral function. By restoring the ability to chew a wider variety of foods, dentures can support better nutrition and quality of life.
Long-term oral health benefits depend on proper fit, regular maintenance, and routine dental exams to monitor tissue changes and the condition of any remaining teeth. In cases where bone preservation is a priority, options such as overdentures or implant-assisted prostheses may offer advantages. Discussing goals and concerns with your dental provider ensures the chosen solution supports both function and facial esthetics.
