
Our Office
Visit Us Online
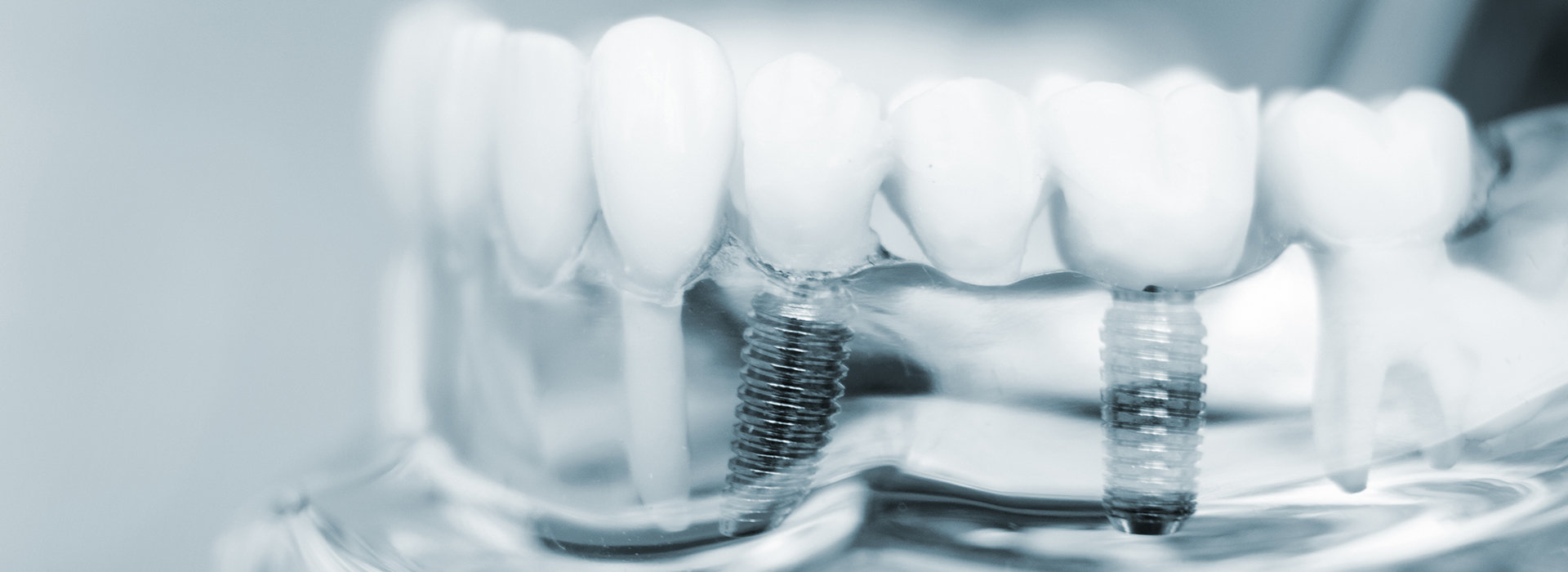
Missing teeth affect more than just appearance — they change how you chew, speak, and maintain long-term oral health. Dental implants are designed to replace both the visible tooth and its supporting root structure, giving patients a stable, natural-feeling restoration. For many people, implants offer a predictable path back to normal function and confidence.
Unlike removable options, implants integrate with jawbone to form a secure foundation for crowns, bridges, or denture attachments. That stability translates into fewer day-to-day restrictions: patients often report easier eating, clearer speech, and less worry about slippage or adhesives. Because implants rely on bone integration rather than adjacent teeth for support, they can preserve surrounding dental structure.
At Frisco Smiles Dentistry, our emphasis is on thoughtful planning and long-term outcomes. We work with each patient to evaluate needs, discuss treatment goals, and map a care path that balances function, aesthetics, and durability.

A dental implant begins with a small, biocompatible post that serves as an artificial root. Once placed and allowed to integrate with the bone, this post acts like the foundation of a natural tooth, supporting a crown or other prosthesis. The result is a restoration that behaves very similarly to a natural tooth in chewing and force distribution.
The restorative component — the crown, bridge, or denture — is crafted to match the surrounding teeth in color and contour. Advanced digital tools and precise lab work help ensure the final restoration looks harmonious and fits comfortably. Because implants transfer chewing forces into the bone, they also help maintain facial structure by protecting against the bone loss that follows tooth loss.
Successful implant care begins with a comprehensive assessment. That includes a review of medical and dental history, oral exam, and imaging to evaluate bone volume and the position of neighboring structures. This planning phase determines whether additional procedures — such as bone grafting — are needed before implant placement.
Surgery to place an implant is typically performed in the dental office and is considered a minor outpatient procedure. Patients receive detailed instructions about anesthesia options and post-op care. Many people tolerate the treatment well and experience manageable recovery when they follow the plan set by the dental team.
After placement, the implant undergoes osseointegration, a natural process in which the bone bonds to the implant surface. Once integrated, the restorative phase begins: impressions or digital scans are used to fabricate the crown, bridge, or denture that will be attached to the implant. In select cases, a temporary restoration may be placed immediately for function and appearance while healing progresses.
Dental implants provide several advantages that affect both oral health and daily life. Because they replace the tooth root, implants help preserve the surrounding bone and support natural facial contours. That preservation reduces the risk of the sunken appearance that can occur over time after tooth loss.
From a functional perspective, implants restore biting power and chewing efficiency. This can make it easier to enjoy a varied diet and maintain proper nutrition. Implants also eliminate many common limitations of removable prostheses: there’s no adhesive to manage, and the risk of slipping when speaking or eating is greatly reduced.
Maintenance is straightforward — implants are cared for with routine brushing, flossing, and professional checkups. They do not decay like natural teeth, but surrounding tissues still need attention to prevent gum disease and ensure longevity.
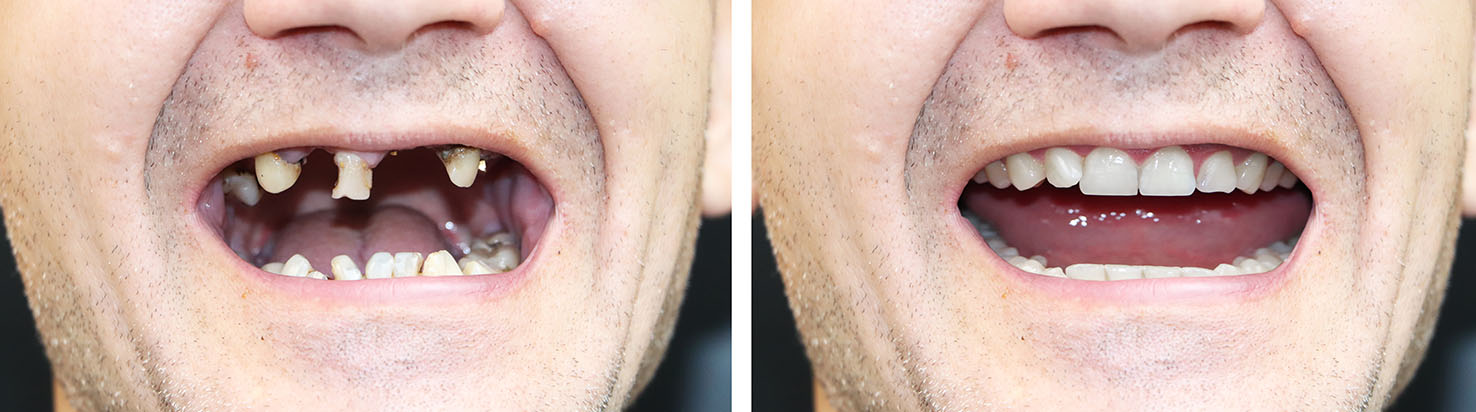
Implant therapy is flexible. A single-tooth implant restored with a crown provides a conservative solution for one missing tooth, avoiding alteration of adjacent teeth. It replaces the lost tooth in both function and appearance while preserving neighboring dental structure.
When several adjacent teeth are missing, an implant-supported bridge uses implants to support multiple replacement teeth without relying on natural teeth for anchorage. This preserves healthy adjacent teeth and delivers more stable chewing compared with removable alternatives.
For patients missing many or all teeth in an arch, a full-arch solution supported by a small number of strategically placed implants can restore a stable, non-removable set of teeth. This approach often allows for immediate temporary teeth followed later by a permanent restoration once healing is complete.
Implant-retained dentures clip or lock onto implants to greatly improve retention and comfort. While the denture may be removable for cleaning, attachment to implants reduces movement and enhances chewing performance compared with conventional dentures.
Candidacy for implants depends on several factors, including overall health, oral hygiene, and the amount of available jawbone. Controlled systemic conditions and good oral care are important for successful outcomes. Imaging and clinical evaluation help determine whether bone grafting is necessary to build a stable foundation for implants.
Bone grafts are commonly used when natural bone volume is insufficient. They provide the support needed for a long-lasting implant by rebuilding the ridge where the implant will be placed. Grafting techniques and materials are well established and tailored to the patient’s anatomy and treatment timeline.
After implant placement, a healing period allows the implant to integrate with the bone. During this time, patients follow post-operative care guidelines to minimize complications: rest, appropriate oral hygiene, and follow-up visits to monitor healing. Once integration is verified, the final prosthesis is attached and function is restored.
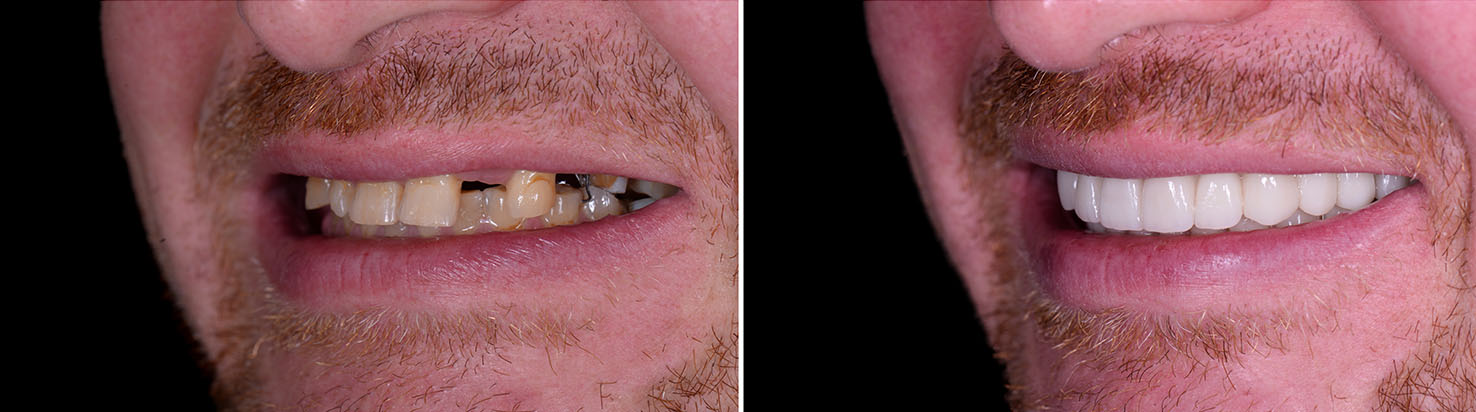
Every implant treatment plan is personalized. We consider your goals for appearance and function, medical and dental history, and lifestyle when recommending the best approach. Clear communication about each step — from planning through restoration and maintenance — helps patients feel informed and confident throughout the process.
Dental implants are a long-term investment in oral health. With careful planning, thorough surgical techniques, and attentive follow-up, they can return reliable function and a natural appearance for many years.
If you’re curious whether implants are the right solution for your smile, our team can review your situation and explain the options. Contact us to learn more and discuss a personalized plan that works for you.
Dental implants are medical-grade posts that replace a missing tooth root and provide a stable foundation for a crown, bridge, or denture. They are typically made from biocompatible materials such as titanium or zirconia that allow the bone to bond to the implant surface. This bonding process, called osseointegration, creates a secure connection that mimics the way a natural tooth root functions.
Once osseointegration occurs, the implant transfers chewing forces into the jawbone much like a natural tooth, which helps restore normal chewing efficiency and speech. The visible restoration is crafted to match the surrounding teeth in color and contour so the result looks and feels natural. Proper planning and precise restorative work are essential to achieve long-term function and aesthetics.
Good candidates for dental implants are generally adults who are in overall good health, maintain reasonable oral hygiene, and have sufficient jawbone to support an implant or are willing to undergo bone grafting when needed. Controlled medical conditions, such as well-managed diabetes, do not automatically disqualify a patient, but they are considered during treatment planning. A thorough evaluation including medical history, dental exam, and imaging determines candidacy and any preparatory steps that may be required.
Lifestyle factors and habits such as tobacco use can affect healing and long-term success, so candidacy discussions include guidance on risk modification. For patients with insufficient bone, grafting or staged approaches can often create a suitable foundation. Ultimately, candidacy is determined on a case-by-case basis with attention to both oral and systemic health.
Treatment begins with a comprehensive assessment that includes a review of medical and dental history, a clinical exam, and diagnostic imaging such as digital x-rays or cone beam CT when appropriate. These records let the dental team evaluate bone quantity and quality, the position of adjacent structures, and the ideal implant placement for both function and aesthetics. When necessary, preliminary procedures such as tooth extractions or bone grafting are planned to create a stable foundation for implants.
Your personalized treatment plan outlines the recommended sequence of care, anesthesia options, expected timelines, and follow-up visits so you know what to expect at each step. At Frisco Smiles Dentistry we emphasize clear communication and collaborative decision-making so patients understand their options and the rationale behind each recommendation. This planning phase is key to predictable outcomes and patient comfort during treatment.
Implant surgery is usually performed in the dental office as a minor outpatient procedure under local anesthesia, conscious sedation, or other comfort options based on the treatment plan. During the procedure, the implant site is prepared and the post is positioned in the bone, after which the site is sutured and allowed to heal. In some cases a temporary restoration is placed to preserve appearance and basic function while healing occurs.
Recovery commonly involves mild swelling and soreness that can be managed with prescribed or over-the-counter medications and by following post-operative instructions. Patients receive specific guidance on oral hygiene, diet, and activity for the initial healing period and return for follow-up visits to monitor osseointegration. Most people tolerate the procedure well and experience progressively improving comfort over the first week or two.
The primary healing period for osseointegration typically ranges from several weeks to a few months, depending on factors such as bone quality, the implant site, and whether grafting was performed. Sites with dense bone often integrate more quickly, while areas that required grafting may need additional time to achieve stable support. Your clinician will schedule follow-up imaging and exams to confirm that the implant has integrated and is ready for the restorative phase.
Once integration is verified, impressions or digital scans are taken to fabricate the final crown, bridge, or denture, and the permanent restoration is attached to restore full function. In select cases immediate provisional restorations are used to provide aesthetics and limited function during healing, but the timing for final restoration is individualized. The complete timeline is discussed during treatment planning so patients have realistic expectations for each phase.
Implant therapy is adaptable to a range of needs, from replacing a single tooth to restoring an entire arch. A single-tooth implant with a crown replaces one missing tooth without altering neighboring teeth and provides a conservative long-term solution. For several adjacent missing teeth, an implant-supported bridge can replace multiple teeth using implants for support instead of relying on natural teeth.
For patients missing many or all teeth, full-arch fixed restorations anchored by a small number of strategically placed implants can provide non-removable replacement teeth with improved stability and comfort. Implant-retained dentures are another option; these removable prostheses attach to implants to reduce movement and improve chewing while still allowing removal for cleaning. Your dentist will recommend the solution that best balances function, aesthetics, and maintenance for your situation.
Because implants replace the root portion of a lost tooth, they transmit chewing forces into the jawbone and stimulate bone maintenance in a way that removable prostheses cannot. This mechanical stimulation helps slow or prevent the bone resorption that commonly follows tooth loss, supporting natural facial contours and reducing the likelihood of a sunken appearance over time. Preserving bone also supports the long-term stability of neighboring teeth and any future restorative options.
Maintaining healthy bone levels contributes to overall oral function and appearance, which is why early assessment and timely replacement of missing teeth are important. When bone loss has already occurred, grafting procedures can rebuild the ridge to support implants and restore a more natural foundation. Thoughtful planning ensures that implant placement not only replaces teeth but also protects the supporting structures that keep a smile healthy.
Daily home care for implants mirrors the practices used to protect natural teeth: thorough brushing, interdental cleaning with floss or brushes, and regular use of any adjunctive tools recommended by your dentist. Avoiding habits that place undue stress on restorations, such as chewing very hard objects, helps protect the prosthesis and underlying implant. Consistent oral hygiene reduces the risk of inflammation around the implant and supports long-term success.
Regular professional checkups and cleanings are critical to monitor the health of implant-supported restorations and the surrounding tissues. Your dental team will assess for signs of peri-implant inflammation and provide targeted cleaning and maintenance protocols as needed. Prompt attention to any changes in comfort, mobility, or gum health helps address issues early and preserve the implant over time.
As with any surgical procedure, implant placement carries potential risks such as infection, delayed healing, or complications involving nearby anatomical structures; however, careful planning and sterile technique minimize these chances. Rarely, issues such as nerve irritation, sinus involvement in the upper jaw, or insufficient integration can occur and are addressed by the clinical team. Patient factors like smoking or poorly controlled systemic conditions can increase risk and are part of the preoperative assessment.
When complications arise, management options range from conservative care and antibiotics to additional surgical interventions such as grafting or implant revision, depending on the specific problem. Close follow-up and early intervention improve the likelihood of resolving complications and achieving a stable outcome. Open communication with your dental team about symptoms and healing progress is essential to manage issues promptly and effectively.
The implant process at Frisco Smiles Dentistry is grounded in comprehensive evaluation, modern diagnostic tools, and individualized treatment planning to align function and aesthetics with each patient’s goals. Digital imaging and precise laboratory work help the team position implants optimally and craft restorations that blend seamlessly with the surrounding dentition. Emphasis on thorough planning reduces surprises and supports predictable outcomes.
The practice combines state-of-the-art technology with patient education and ongoing maintenance to protect investments in oral health, and the team prioritizes follow-up care to monitor healing and long-term tissue health. By focusing on prevention, clear communication, and tailored maintenance protocols, Frisco Smiles Dentistry helps patients achieve durable, comfortable results that support overall oral wellness.
