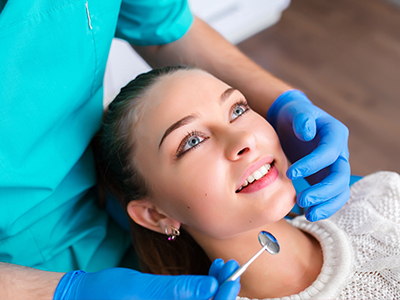
Our Office
Visit Us Online
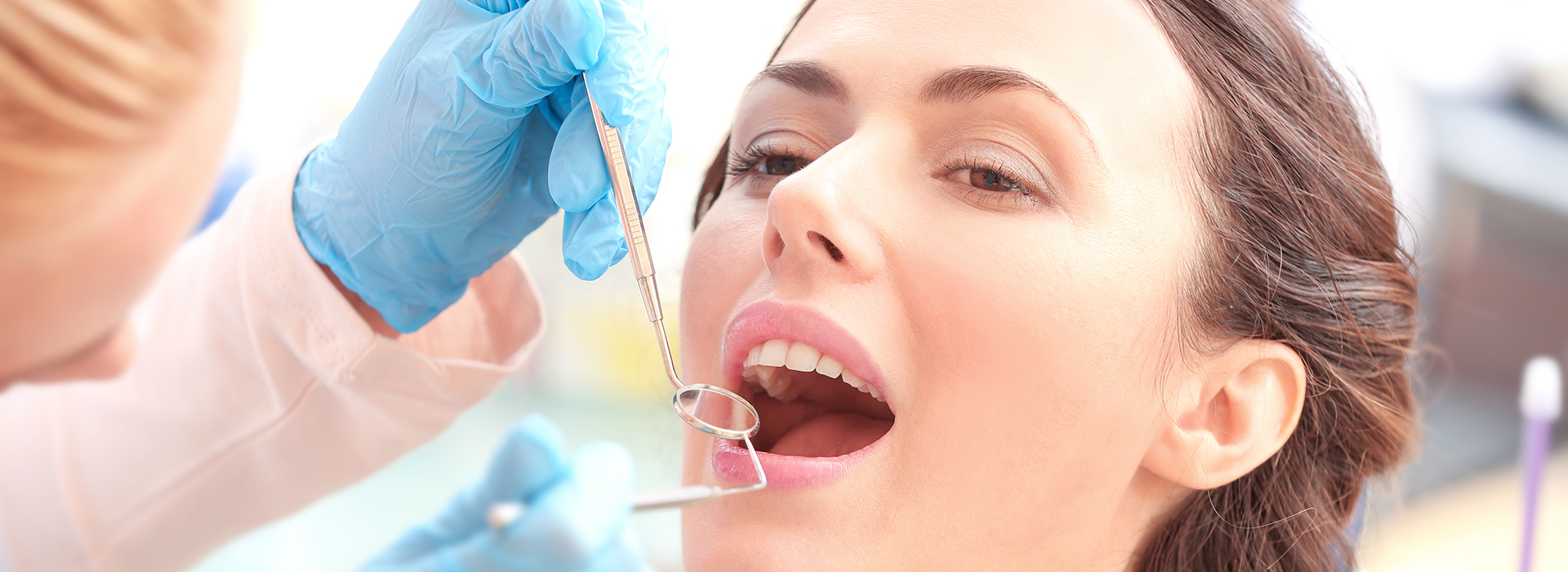
Gum disease is the leading cause of tooth loss for adults, yet it often develops quietly and can be managed or prevented with timely care. Research shows a large portion of adults show signs of periodontal disease by middle age, but the condition is not inevitable. At the office of Frisco Smiles Dentistry, we focus on helping patients protect their gums and preserve the supporting structures that keep teeth healthy and functional.
Periodontal disease begins when bacteria in dental plaque accumulate along the gumline and below the gums. The immune response to those bacteria creates inflammation that, over time, damages the tissues that attach teeth to bone. Early stages are limited to the gum tissue; later stages affect connective tissue and bone.
Because early gum disease can be subtle, many people do not notice symptoms until the condition is more advanced. That’s why regular dental checkups and professional cleanings are essential — they let a clinician catch changes that are not yet obvious to you and recommend steps to stop progression.
Understanding the mechanics of periodontal disease — bacterial accumulation, inflammatory response, and tissue breakdown — helps patients appreciate why daily home care and professional intervention work together to protect long-term oral health.
Noticing early warning signs makes a significant difference in prognosis. While the disease can be painless at first, a number of visible and functional changes often indicate gum inflammation or advancing disease. Early recognition allows for less invasive treatment and better preservation of support structures.
Common signs to watch for include:
Red, swollen, or tender gums
Bleeding during brushing or flossing
Receding gumline or visible root surfaces
Increased tooth sensitivity to temperature
Persistent bad breath or an unpleasant taste
Looseness in one or more teeth
New gaps between teeth or a changing bite
Changes in the fit of partial dentures
Pus or discharge near the gumline
Pain when chewing or biting

Oral health doesn't exist in isolation. Chronic inflammation in the mouth can influence overall health and has been associated with conditions such as cardiovascular disease, diabetes management, and respiratory illness. Controlling gum inflammation is therefore not only about preserving teeth — it's about supporting broader health goals.
Regular periodontal assessments are part of a preventive strategy that helps identify risks early and coordinate care with other healthcare providers when needed. For patients with systemic conditions, attention to periodontal health can be particularly important for reducing potential complications.
Prevention, early detection, and maintenance form the backbone of effective periodontal care. By addressing problems while they are still mild, the need for more invasive treatments can often be avoided.
Gingivitis is the earliest, reversible form of gum disease. It is characterized by gum redness, swelling, and bleeding but without loss of the connective tissue or bone that anchor teeth. When identified at this stage, simple professional and home-based measures typically restore gum health.
Treatment for gingivitis centers on removing plaque and tartar, improving daily oral hygiene habits, and establishing a schedule of professional cleanings. These steps reduce the bacterial load and calm inflammation, allowing the gums to heal and reattach to tooth surfaces.
Commitment to consistent brushing, flossing, and periodic dental visits is key. With these measures most cases of gingivitis can be resolved and monitored so that progression to more destructive disease is prevented.

If inflammation persists, gingivitis can progress into periodontitis, a stage where the connective tissues and bone that support teeth become compromised. This results in deepened pockets around teeth, gum recession, and potential bone loss — changes that require active intervention to control.
The clinical focus with periodontitis is to stop tissue destruction, reduce pocket depths so that effective home care is possible, and, when appropriate, restore lost tissue. Each case varies in severity, and treatment plans are tailored to tissue involvement, overall health, and patient goals.
Although periodontitis is more complex than gingivitis, modern periodontal therapies can stabilize the condition and, in many cases, promote regeneration of affected tissues when clinically indicated.
Every periodontal treatment plan starts with a thorough assessment: a clinical exam, pocket depth measurements, and review of medical history and oral hygiene practices. This evaluation identifies the stage of disease and any factors that may influence treatment choices.
From there, we discuss personalized options designed to restore and maintain periodontal health. The aim is to select the least invasive approach that will achieve long-term stability, while also considering the patient's preferences and overall oral care routine.
We use a combination of proven techniques and technology to manage periodontal conditions and continuously reassess progress to ensure outcomes are maintained over time.
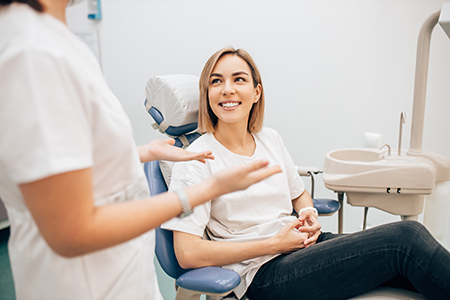
When disease is detected early or is limited in scope, non-surgical options often succeed in halting progression. These methods focus on removing plaque and hardened deposits from below the gumline and smoothing root surfaces to discourage bacterial recolonization.
Scaling and root planing are core procedures in conservative care. By mechanically disrupting biofilm and calculus beneath the gums, inflammation is reduced and pockets can shrink. Adjunctive antimicrobial therapies may be used when indicated to help control infection.
These approaches emphasize improved home care and ongoing maintenance visits to keep the disease under control and minimize the chance of recurrence.
If non-surgical treatment does not achieve the necessary improvement, the clinical team will discuss additional options that can address deeper tissue involvement.
For pockets that are too deep to clean effectively with non-surgical methods, or when significant tissue or bone loss has occurred, surgical treatment can provide access for thorough cleaning and correction. Surgery aims to reduce pocket depth, reshape damaged tissue, and create conditions suitable for healing.
Flap procedures allow clinicians to lift the gum tissue, remove deposits from root surfaces, and recontour bone if necessary before suturing the tissue back in a healthier position. In many cases, regenerative materials or grafts are used to encourage bone and soft-tissue repair.
Contemporary tools such as lasers may be used selectively for certain periodontal tasks, including reducing pocket depth and managing inflamed tissue, depending on the clinical situation and practitioner judgement.
With appropriate surgical care followed by meticulous maintenance, the risk of further tooth-support loss can be reduced and oral function preserved.
If you have noticed any signs of gum disease or are concerned about changes in your gums or bite, we encourage you to reach out for an evaluation. Early action makes a measurable difference in outcomes.
At Frisco Smiles Dentistry, our goal is to help patients maintain healthy, stable gums through evidence-based care and ongoing support. Contact us to learn more about periodontal options and to schedule an evaluation if you have questions about your gum health.
Gum disease begins when bacterial plaque accumulates along the gumline and below the gums, creating a biofilm that irritates soft tissues. The body’s immune response to that bacterial challenge produces inflammation, which over time can damage the connective tissues that attach teeth to bone. Without interruption through professional care and daily hygiene, this process can progress from reversible inflammation to deeper tissue and bone loss.
Factors such as inadequate brushing and flossing, tobacco use, certain medications, and some medical conditions increase the risk of progression. Regular dental exams help identify early signs and let clinicians intervene before significant structural damage occurs. Understanding the biological steps from plaque to inflammation helps patients see why both home care and clinical treatment are necessary.
Early gum disease is often subtle but commonly shows as red, swollen, or tender gums and bleeding during brushing or flossing. Patients may also notice persistent bad breath, increased tooth sensitivity, or a receding gumline that exposes darker root surfaces. These signs do not always cause pain, so they can be easy to dismiss if not evaluated by a dental professional.
Paying attention to small changes in your mouth allows for less invasive treatment and better long-term outcomes. If you notice any of these symptoms, mention them at your next appointment so the clinician can perform targeted assessments. Timely detection typically means simpler therapy and a greater chance of full recovery of gum health.
Diagnosis begins with a thorough clinical exam that includes measuring pocket depths around each tooth, checking for gum recession, and assessing mobility and bleeding on probing. A review of your medical history and risk factors, as well as radiographs when indicated, helps determine how far the disease has progressed and whether bone loss is present. This comprehensive evaluation establishes a baseline for treatment decisions and ongoing monitoring.
Additional considerations such as tobacco use, diabetes status, and certain medications are incorporated into the assessment because they influence treatment choices and prognosis. The clinician will discuss findings and explain staging and grading of disease when applicable. Clear documentation and regular reassessment support personalized care and long-term stability.
Treatment for gingivitis and early periodontal disease focuses on removing plaque and calculus and reducing inflammation so the gums can heal. Professional cleanings, improved daily oral hygiene, and targeted antimicrobial measures are the primary interventions used to restore healthy gum tissue. When found early, these conservative steps are often effective at reversing disease and preventing progression.
After initial therapy, a personalized maintenance schedule is established to sustain results and monitor for recurrence. Education about brushing technique, interdental cleaning, and risk-factor modification complements clinical care. Ongoing professional cleanings and periodic reassessment help ensure that early disease remains controlled.
Surgical or regenerative therapy is considered when pockets are too deep to be cleaned effectively with non-surgical methods or when significant soft-tissue or bone loss has occurred. Procedures such as flap surgery provide direct access to root surfaces for thorough debridement and allow for recontouring of bone or placement of grafts when regeneration is appropriate. The goal of these interventions is to reduce pocket depths, stop disease progression, and create conditions that support effective home care.
Regenerative techniques may use bone grafts, barrier membranes, or biologic agents to encourage new attachment and bone fill in selected cases. Contemporary approaches are chosen based on the specific pattern of tissue loss, overall health, and the patient’s restorative and esthetic goals. With proper surgical care followed by diligent maintenance, many patients achieve long-term stability of the dentition.
Scaling and root planing are non-surgical procedures that remove plaque and hardened deposits from below the gumline and smooth root surfaces to discourage bacterial recolonization. The clinician typically performs these procedures under local anesthesia to enhance comfort and may treat one or more quadrants at a time depending on the extent of disease. After treatment, inflammation usually subsides over several weeks as the tissues heal and reattach to cleaned root surfaces.
Patients can expect some sensitivity or mild soreness for a few days and are advised to follow post-operative care instructions to support healing. A follow-up visit is scheduled to reassess pocket depths and evaluate response to therapy, and additional treatment may be recommended if pockets do not resolve. Consistent home care and supportive maintenance are essential to preserve the benefits of scaling and root planing.
Oral hygiene and home care are foundational to both treating and preventing periodontal disease because daily removal of plaque dramatically reduces the bacterial load that drives inflammation. Effective routines include twice-daily toothbrushing with a suitable technique, daily interdental cleaning with floss or proxabrushes, and attention to areas where plaque tends to accumulate. Patients who adopt and maintain these habits reduce the likelihood of disease progression and the need for more extensive interventions.
In addition to mechanical cleaning, lifestyle factors such as smoking cessation, good glycemic control for people with diabetes, and regular professional care support periodontal health. The clinical team provides individualized coaching on techniques and tools that fit each patient’s dexterity and oral anatomy. A partnership between patient and clinician is the most reliable way to achieve and sustain healthy gums.
Chronic inflammation in the mouth can have effects beyond the teeth and gums and has been associated with systemic conditions such as diabetes management, cardiovascular health, and certain respiratory issues. While associations do not imply direct causation in every case, controlling oral inflammation can help reduce overall inflammatory burden and support general health goals. For patients with medical conditions, periodontal care is often an important component of comprehensive health management.
Because oral and systemic health are interconnected, clinicians may coordinate care with a patient’s physician or specialist when underlying conditions could influence treatment choices. Maintaining periodontal health can contribute to improved quality of life, better nutrition, and more predictable outcomes for other therapies. Regular communication between dental and medical providers helps ensure safe, effective care tailored to the whole person.
Every treatment plan starts with a detailed assessment of periodontal status, medical history, risk factors, and the patient’s goals for function and appearance. From that foundation, clinicians select the least invasive options that will achieve long-term stability, balancing non-surgical and surgical approaches as indicated by tissue involvement. Treatment sequencing, supportive therapies, and maintenance intervals are determined by the disease stage and the patient’s ability to maintain home care.
Individual factors such as smoking, medications, systemic diseases, and restorative needs are taken into account when planning care. The practice emphasizes patient education so individuals understand the rationale for recommended steps and their role in successful outcomes. When appropriate, clinicians will discuss regenerative options or multidisciplinary referrals to address complex restorative or esthetic concerns; at Frisco Smiles Dentistry this collaborative approach helps align treatment with each patient’s priorities.
You should schedule an evaluation if you notice bleeding, swelling, persistent bad breath, increased tooth sensitivity, loose teeth, or any change in the fit of partial dentures or bite. Routine periodontal assessments are also recommended at regular dental checkups so clinicians can detect early changes even when symptoms are absent. Early evaluations increase the chance of successful, less invasive treatment and better long-term results.
To schedule an evaluation at Frisco Smiles Dentistry, call our office at (469) 212-9064 for new patients or (469) 294-4239 for existing patients. Our office is located at 2955 Eldorado Pkwy, Suite 110, Frisco, TX 75033, and we offer appointment times designed to fit weekday schedules. If you are experiencing pain or acute changes, contact the office promptly so a clinician can advise on next steps.
